Laser and Surgical Options for Open-Angle Glaucoma
Please see the previous two blogs, Glacuoma and Medical Therapy for Open-Angle Glacuoma, for more information on the topic.
Primary open angle glaucoma (POAG) is a condition in which elevated eye pressure damages the optic nerve. Lowering of eye pressure usually slows the progression of the disease.
Topical medications (drops) are the mainstay of glaucoma therapy. These medications work either by decreasing aqueous production or increasing aqueous outflow. The majority of patients with glaucoma can be effectively managed with drops.
When topical therapy proves to be inadequate, laser or surgery may be considered.
Laser Treatment


Trabeculoplasty
Selective laser trabeculoplasty (SLT) uses a 532nm Nd:YAG laser that delivers energy to pigmented cells in the trabecular meshwork, the drainage system of the eye. This improves aqueous outflow and is effective in lowering eye pressure in most patients. The benefit is comparable to the use of one topical glaucoma medication, causing a 20-25% reduction in intraocular pressure.
Effects of SLT may wane over time, with up to half of patients requiring further treatment within 5 years. SLT may be repeated if necessary.
SLT is an effective supplement or alternative to drops for the treatment of glaucoma. SLT can be performed as an initial therapy in select cases.
Elevated eye pressure is a rare complication observed immediately following SLT.
Argon laser trabeculoplasty (ALT) is similar to SLT, but uses a heat based laser to photocoagulate tissue.
Ciliary Body Ablation
Ciliary body ablation (CBA) is a technique in which the aqueous producing cells of the ciliary body are ablated, or destroyed, by heat (laser) or cold (cryotherapy) thereby reducing aqueous production and lowering intraocular pressure. The procedure can be performed transsclerally or endoscopically.
Transscleral cyclophotocoagulation (TS-CPC) involves placing a probe against the eye to deliver laser energy to the ciliary processes. TS-CPC is usually performed on advanced cases of neovascular glaucoma when visual potential is limited.
Complications of TS-CPC include transient pain, inflammation, and hypotony.
Incisional Surgery


Trabeculectomy
Trabeculectomy is a surgical procedure that involves the creation of a path from the scleral to the trabecular meshwork through an external incision. This allows aqueous to leak out of the anterior chamber into the subconjunctival space, forming a bleb, or bubble-like blister of fluid under the conjunctiva. The eye pressure often lowers markedly, and the patient can usually stop most, or all of their glaucoma drops. Antifibrotic agents such as mitomycin C and 5-fluorouracil can be applied intraoperatively to lessen scarring and subsequent surgical failure.
Over time, the bleb may scar and the surgery fail. Success rates vary, but range from 31-88%.
Complications from trabeculectomy surgery include hypotony, maculopathy, and infection. Some complications may be severe and vision threatening, even with appropriate therapy.
Tube-Shunt Surgery
Tube-shunts are surgically implanted devices that allow aqueous to drain through a tube to an endplate under the conjunctiva. They are often utilized in advanced and complicated cases such as neovascular or uveitic glaucoma. Tube-shunts are also a viable alternative to trabeculectomy for medically uncontrollable POAG. These devices are available in different sizes, materials, and design. Two commonly used tube-shunts are the Ahmed Glaucoma Valve and the Baerveldt Glacuoma Implant.
Complications of tube-shunt surgery include hypotony and infection. If the tube contacts the cornea, corneal edema may occur. Erosion of the tube or plate through the conjunctiva has been reported, but the risk is reduced when donor tissue is used to cover the device during surgery.
Minimally Invasive Glaucoma Surgery
Minimally invasive glaucoma surgery (MIGS) refers to a group of surgical procedures that share the following features:
• Ab interno approach through a microincision in the cornea
• Minimal trauma
• Efficacy
• High safety profile
• Rapid recovery


Micro-Stent Surgery
Micro-stent surgery is a technique in which a small device is implanted to lower eye pressure by increasing outflow. Four implants have been developed. They share the advantage of less tissue disruption over traditional incisional surgery, shorter surgical times, and potentially lower risk profiles.
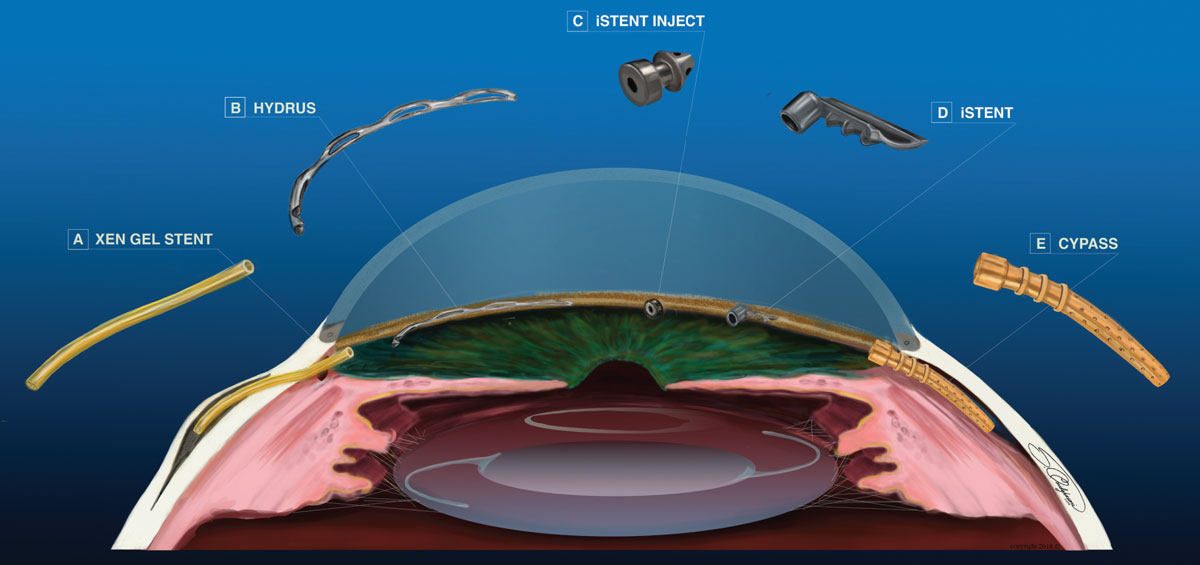
iStent was the first FDA-approved MIGS device. This L-shaped stent is inserted into Schlemm’s canal, with the neck extending into the anterior chamber, allowing aqueous to flow more freely. The newest version of the iStent is the iStent inject. This system uses a single-use injector to implant two titanium stents into the trabecular meshwork allowing aqueous to flow from the anterior chamber into Schlemm’s canal.
Hydrus Microstent, a device made of a nickel-titanium alloy, is inserted into Schlemm’s canal to establish outflow.
CyPass Micro-Stent is a polyamide tube inserted into the supraciliary space between the ciliary body and the sclera, allowing for suprachoroidal aqueous outflow.
XEN Gel Stent is a collagen-derived gel device inserted to create a pathway between the anterior chamber and subconjunctival space.
There are numerous other micro-shunt devices under development which may be available in the future.
Risks associated with micro-stent surgery include failure to implant the device, and damage to iris or cornea during implantation. Risks seen with traditional glaucoma surgeries, such as infection or hypotony, are much lower with MIGS techniques.
Alert
The FDA determined during a post approval study that CyPass implants are associated with loss of the endothelial cells of the cornea. As endothelial cell loss is associated with the potential for development of corneal edema and vision loss, Alcon withdrew the implant from the market.
It is not yet known if any other devices will experience similar problems in post-approval studies. The FDA is currently monitoring the data.
Trabeculectomy/Trabeculotomy
Trabectome is an electrocautery device used to perform a partial trabeculectomy. Electrocautery, irrigation, and aspiration are used to selectively ablate the trabecular meshwork and the inner wall of Schlemm’s canal. Complications include hyphema and synechiae.
Kahook Dual Blade is a single-use knife with two parallel blades designed to remove a strip of the trabecular meshwork and the inner wall of Schlemm’s canal to improve outflow. Hyphema is a common complication.
Gonioscopy-assisted transluminal trabeculotomy (GATT) creates a 360° trabeculotomy. The procedure is performed through two 1.0 mm corneal incisions and employs either a microcatheter or Prolene suture that is threaded through the circumference of Schlemm’s canal and then pulled through to unroof the trabecular meshwork. TRAB 360 is a device designed to perform GATT using only one corneal incision. The most common complication is hyphema.
Canaloplasty
Ab interno canaloplasty (ABiC) is perfomed through a single corneal incision and involves the 360° viscodilation of Schlemm’s canal. As with GATT, a microcatheter device is advanced through Schlemm’s canal. Instead of pulling the microcatheter to cut the TM, the surgeon extracts it as viscoelastic is gently injected into Schlemm’s canal. This viscodilation breaks adhesions within Schlemm’s canal, stretches the trabecular plates and creates microperforations within the inner wall. It also improves outflow by irrigating collector channel blockages.
Cyclophotocoagulation
Endoscopic cyclophotocoagulation (ECP) is the endoscopically performed technique of ciliary body ablation mentioned previously. ECP utilizes a fiberoptic viewing system and laser probe inserted into the eye through an incision to visualize and treat the ciliary processes. ECP may be performed as a stand-alone procedure, or combined with another eye surgery (cataract or retinal procedure).
Temporary inflammation is common following ECP. Traumatic injury to the iris has been reported. Due to the invasive nature of all surgical procedures, infection or hemorrhage may occur, but are rare.
From the Expert…
In the past, the diagnosis of glaucoma meant progressive vision loss, toxic medications, invasive surgery, and the risk for permanent blindness. Modern medical advances have greatly improved the care and visual outcomes for patients with the disease.
Today, glaucoma management involves careful, non-invasive monitoring, well tolerated drops, effective laser treatment, and occasionally, incisional surgery. The standard of care is well established and usually leads to control of the disease and a favorable outcome.
ADDITIONAL RESOURCES
American Academy of Ophthalmology Glaucoma Panel. Preferred Practice Pattern®Guidelines. Primary Open-Angle Glaucoma. San Francisco, CA: American Academy of Ophthalmology; 2015. Available at: www.aao.org/ppp.
Glaucoma. American Academy of Ophthalmology. EyeWiki. https://eyewiki.aao.org/Category%3AGlaucoma. Accessed August 29, 2019.
Summary Benchmarks for Preferred Practice Pattern® Guidelines. Glaucoma. American Academy of Ophthalmology; 2018.
Manasses, DT and Au, L. The New Era of Glaucoma Micro-stent Surgery. Ophthalmology and Therapy 2016;5:135-146.
Potential Eye Damage From Alson CyPass Micro-Stent Used to Treat Open-Angle Glaucoma: FDA Safety Communication. https://www.fda.gov/medical-devices/safety-communications/potential-eye-damage-alcon-cypass-micro-stent-used-treat-open-angle-glaucoma-fda-safety. Accessed October 1, 2019.