Medical Therapy for Open-Angle Glaucoma
Please see the previous blog, Glacuoma, for more information on the topic.
In a healthy eye, aqueous fluid is produced by the ciliary body, flows through the pupil, and drains through the trabecular meshwork.
In glaucoma, the optic nerves are damaged by elevation of eye pressure. Accordingly, therapy is focused on lowering the intraocular pressure (IOP).
The mainstay of open-angle glaucoma treatment is topical medication, in the form of eye drops. These medicines work by decreasing fluid (aqueous) production or facilitating its drainage. Sometimes, only one medication may be required to adequately reduce a patient’s IOP. Other times, multiple medications are required.
Beta-Adrenergic Antagonists
Beta-adrenergic antagonists (β-blockers) work by inhibiting the aqueous production of the ciliary body. Timoptic (timolol maleate) is a frequently prescribed beta blocker agent and is used once daily in the morning or sometimes twice a day. Other non-selective β-blockers include Betagan (levobunolol), Betimol (timolol hemihydrate), and Ocupress (carteolol). Typically, IOP is reduced by 20-30% with β-blockers.
Contraindications to β-blockers include chronic obstructive pulmonary disease (COPD), asthma, congestive heart failure, or cardiac arrythmia, as they can make these conditions worse. A selective β-blocker such as Betoptic S (betaxolol) can sometimes be used safely in these patients, but is typically less effective than a non-selective β-blocker.
In glaucoma, the flow of aqueous fluid becomes impaired, much like a sink that cannot drain, leading to increased pressure in the eye.
Prostaglandin Analogues
Prostaglandin analogues work by increasing aqueous outflow. Typically, pressure is lowered by 25-33%. Lumigan (bimatoprost), Xalatan (latanoprost), Travatan Z (travoprost), Zioptan (tafluprost), and Vyzulta (latanoprostene bunod) are examples of these agents. These medications are taken once daily, at bedtime.
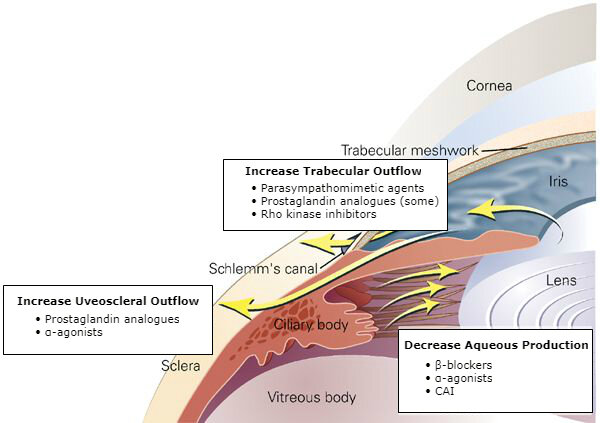
Medical therapies for open-angle glaucoma
Contraindications to prostaglandin analogues include ocular herpetic infection, recent eye surgery, uveitis, or macular edema, as they can exacerbate these conditions.
Complications of prostaglandins include a red, injected eye, and darkening of the lids, lashes, and iris.
Carbonic Anhydrase Inhibitors
Carbonic anhydrase inhibitors (CAI) suppress aqueous production, thereby lowering ocular pressure. Most commonly they are administered topically three times daily, but can also be administered orally. Trusopt (dorzolamide HCl) and Azopt (brinzolamide) are examples of the topical form. Diamox (acetazolamide) and Neptazane (methazolamide) are examples of the oral form. Topical CAI have been shown to reduce IOP by 15-20%.
CAI are often utilized as a second-line treatment, supplementing either β-blockers or prostaglandin analogues.
Contraindications of CAI include sulfonamide allergy, kidney stones, and sickle cell anemia. Orally, they often cause tingling in the fingers and lower blood potassium levels, particularly for patients taking a diuretic.
Alpha-Adrenergic Agonists
Alpha-adrenergic agonists (α-agonists) lower pressure primarily by decreasing aqueous production. Alphagan P (brimonidine tartrate) and Iopidine (apraclonidine HCl) are examples of such agents. They are usually dosed three times per day, and cause a reduction of 20-25% in IOP.
α-agonists should be used with caution in patients with severe cardiovascular disease or stroke, and is contraindicated for those on MAOI therapy. Systemic absorption can be limited by nasolacrimal duct occlusion for a few minutes following administration.
Complications of α-agonist use include allergic reaction in about 20% of patients.
Parasympathomimetic Agents
Parasympathomimetic agents lower pressure by facilitating aqueous outflow. Pilocarpine is the most commonly prescribed. Another available medication is carbachol. These medicines are used infrequently as side effects occur relatively often. They include induced myopia (near-sightedness), headache, and poor night vision. Furthermore, risk for cataract progression and retinal detachment have been reported.
Rho Kinase Inhibitors
Rho kinase inhibitors such as Rhopressa (netarsudil), work by increasing aqueous outflow. The medication is dosed once daily, at bedtime. This is the newest class of glaucoma agent, and has only been available since April 2018.
Side effects of rho kinase inhibitors may include redness, corneal deposits, stinging, and subconjunctival hemorrhage.
Combination Agents
Combination drops are an option for patients who require more than one type of medication. By requiring less daily drops, they increase patient compliance. Available combination drops include Cosopt (dorzolamide HCl and timolol maleate), Combigan (brimonidine tartrate and timolol maleate), and Simbrinza (brinzolamide and brimonidine tartrate).
From the Expert…
Glaucoma is a disease in which elevated eye pressure damages sensitive neurons in the optic nerve. Treatment is focused on lowering the eye pressure, the most modifiable risk factor.
The mechanism of action of glaucoma medications are either a lowering of aqueous production or an increase in aqueous drainage.
The most common drugs as first line therapy are prostaglandin analogues which facilitate aqueous drainage or β-blockers which lower aqueous production. These medications, given their complimentary effects, work well together.
Carbonic anhydrase inhibitors and alpha-adrenergic agonists are usually added in more severe and poorly responsive cases.
Combination drops are available which increase convenience and compliance.
Remember, glaucoma drops are only effective when taken as prescribed. Patient compliance is critical for a successful outcome.
ADDITIONAL RESOURCES
American Academy of Ophthalmology Glaucoma Panel. Preferred Practice Pattern®Guidelines. Primary Open-Angle Glaucoma. San Francisco, CA: American Academy of Ophthalmology; 2015. Available at: www.aao.org/ppp.
Glaucoma. American Academy of Ophthalmology. EyeWiki. https://eyewiki.aao.org/Category%3AGlaucoma. Accessed August 29, 2019.
Summary Benchmarks for Preferred Practice Pattern® Guidelines. Glaucoma. American Academy of Ophthalmology; 2018.