Cystoid Macular Edema


Pseudophakic cystoid macular edema (CME) is a condition in which postsurgical inflammation leads to macular swelling. Surgical removal of the cataract causes the release of inflammatory mediators such as vasoendothelial growth factor (VEGF) and prostaglandins. These mediators cause the parafoveal blood vessels to become leaky. The leaked serum collects in cystoid spaces within the macula. This leads to vision loss, as a swollen macula cannot see well.
Symptoms
Patients with CME will often notice vision loss following a period of improved vision after cataract extraction. The central vision becomes blurry, while peripheral vision remains unchanged. The edema may cause a hyperopic shift.
Evaluation
Biomicroscopic examination of the macula shows loss of the foveal depression and swelling within the macula.

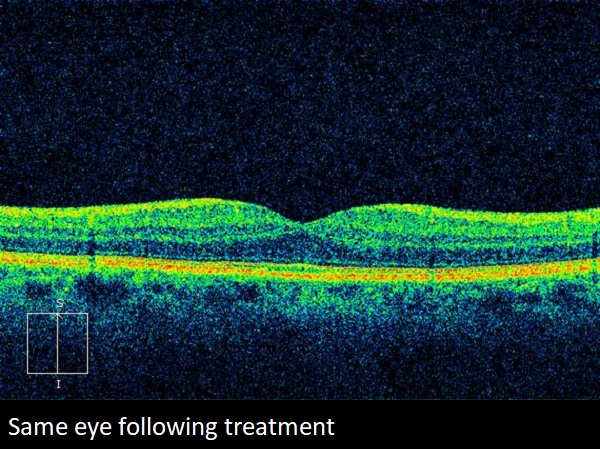
Optical coherence tomography (OCT) uses a laser to image the macula in cross section. This test demonstrates intraretinal cystic spaces and is very sensitive for detecting the disease.
Fluorescein angiography is a photographic test of dye leakage in the retina. In CME, dye pools in the cystic spaces and becomes detectable to the physician. The optic nerve, which is also affected, leaks the dye.
Risk Factors
CME may occur in completely uneventful cataract surgery. It is more common in patients with a history of diabetes, retinal vein occlusion, epiretinal membrane, or vitreoretinal traction.
Topical prostaglandin analogues such as latanoprost, bimatoprost, and travoprost have been shown to increase the risk of CME following ocular surgery.
Complications of cataract surgery such as capsular rupture or retained lens fragments are associated with an increased incidence of CME.
Treatment
Topical steroids and non-steroidal anti-inflammatory (NSAID) drugs are the mainstay of therapy for CME. Diclofenac, ketorolac, bromfenac, and nepafenac are commonly prescribed NSAIDs. They are also used prophylactically to prevent the disease.
If CME persists in spite of topical therapy, steroids can be injected next to (sub-tenons) or into (intravitreal) the eye.
Anti-VEGF injections (Avastin, Eylea, Lucentis) into the vitreous have been shown to improve edema and vision in patients with refractile CME.
Surgical intervention may be necessary to cause resolution of the CME. Vitreal adhesions to the corneal wound, iris, and macula are released. Any residual cataract fragments, which are inflammogenic, are removed. Repositioning of the lens implant may be beneficial.
Complications
Treatment for CME is usually safe and effective. Steroids may cause elevated eye pressure which can induce glaucoma. This usually reverses with cessation of the medication.
Complications of vitrectomy surgery for CME are uncommon, but include shifting of the lens implant, hemorrhage, infection, and retinal detachment.
Prognosis
The outcome of patients with CME is usually quite good. The majority of patients have a full recovery of vision. In chronic and recalcitrant cases, the vision may be permanently diminished.
From the Expert…
All incisional surgery requires inflammation to promote wound healing and recovery. In the eye, these inflammatory messengers cause retinal and optic nerve blood vessels to become leaky. The leaking fluid collects in cystoid spaces in the macula. This leads to CME and subsequent decline in vision.
The occurrence of CME has declined with refinement in cataract extraction surgical technique. Still, even with perfectly performed surgery, CME may occur. Fortunately, treatment for CME is quite effective and the majority of patients experience improvement in their vision.
Additional Resources
Lally DR and Shah CP. Pseudophakic Cystoid Macular Edema. Review of Ophthalmology. Published 5 March 2014. https://www.reviewofophthalmology.com/article/pseudophakic-cystoid-macular-edema . Accessed October 3, 2019.
Yonekawa Y, Eliott D, Kim I. Pseudophakic Cystoid Macular Edema (Irvine-Gass Syndrome). American Academy of Ophthalmology. EyeWiki. https://eyewiki.org/Pseudophakic_Cystoid_Macular_Edema_(Irvine-Gass_Syndrome). Accessed October 3, 2019.
Grzybowski A, Sikorski BL, Ascaso FJ, Huerva V. Pseudophakic cystoid macular edema: update 2016. Clinical Interventions in Aging 2016;11:1221-1229.
Guo S et al. Management of pseudophakic cystoid macular edema. Survey of Ophthalmology 2015;60:123-137.
