Retinal Detachment
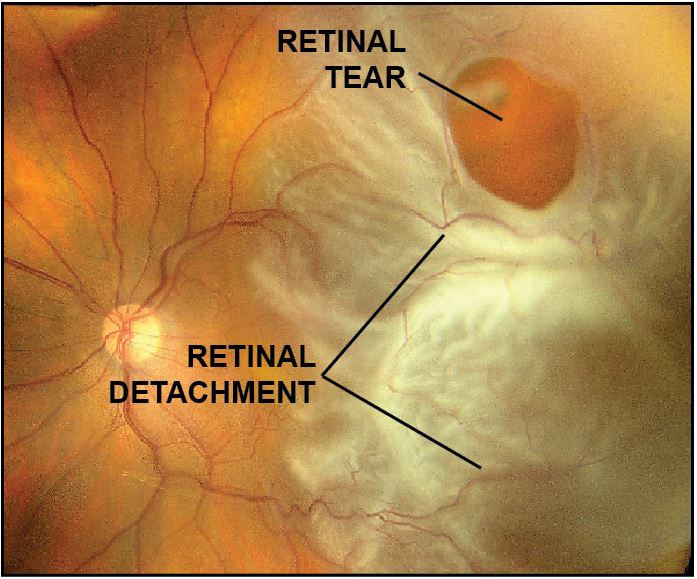
Retinal detachment is a condition in which the retina separates from the back wall of the eye. Most retinal detachments occur following a retinal tear, which allows fluid to pass from the vitreous into the subretinal space.


Symptoms
Symptoms of retinal detachment may include flashes, floaters, or a dark curtain that causes loss of peripheral or central vision.
Evaluation
A complete ocular examination, including a dilated fundus examination, is indicated for every patient with complaints of flashes, floaters, or a dark curtain.
Fundus photography is useful to document the location of retinal tears and extent of retinal detachment.
Ultrasonography may be performed to determine if the retina is detached, especially if the view is obscured by vitreous hemorrhage.
Optical coherence tomography (OCT) can be performed to evaluate for the presence of subretinal fluid and epiretinal membrane.
Treatment



Scleral buckling is a surgical procedure in which a piece of soft silicone material is sewn against the outside wall of the eye, creating an indentation which closes the retinal defect that caused the detachment. The surgeon may also drain accumulated fluid behind the retina. Laser or freezing therapy is then used to seal the retina back into place once it is reattached. The scleral buckle stays in place permanently and does not harm the eye.
Pars plana vitrectomy uses a microscopic cutting instrument to remove the vitreous gel present inside the eye. The fluid that created the retinal detachment is then drained through the existing retinal tear or a retinotomy created by the surgeon, thereby reattaching the retina. A temporary gas bubble holds the retina in position as laser or freezing treatment seals the retina to the eye wall.
Pneumatic retinopexy involves an expansile gas bubble injected into the vitreous cavity which closes the retinal tear and allows reabsorption of the subretinal fluid. A laser or freezing therapy is used to seal the retina to the eye wall. The gas bubble is then slowly absorbed.
Complications
Possible surgical complications may include:
Persistent retinal detachment/retinal re-detachment
Glaucoma
Cataract
Preretinal fibrosis
Hemorrhage
Infection
Accurate diagnosis and effective treatment of surgical complications can usually lead to a successful result.
From the Expert…
Retinal detachments are an ocular emergency. When the retina detaches from the eye wall, it no longer sees normally. Surgical repair is indicated. Vitrectomy, scleral buckle, or pneumatic retinopexy are the treatment modalities most frequently utilized.
In my experience, most detachments are best corrected with vitrectomy. Other surgeons may prefer pneumatic retinopexy or scleral buckle. The surgical technique used is selected by the surgeon and should be tailored to the individual eye based on a detailed preoperative examination of the retina and vitreous.
Acute macula-on detachments are usually fixed within one or two days. Surgical repair of peripheral detachments that do not threaten the central macula can sometimes be delayed. Chronic detachments, or those in which the macula is detached, can usually wait a few days to a week or two.
A successful outcome depends on timely and effective surgical intervention, as well as diligent follow-up examinations and correction of any complications which may occur.
Additional Resources
American Academy of Ophthalmology Committee on Ophthalmic Procedure Assessment. The Repair of Rhegmatogenous Retinal Detachments. Ophthalmology 1996;103:1313-1324.
Patel, S. Retinal Detachment. American Academy of Ophthalmology. Eye Wiki. https://eyewiki.aao.org/Retinal_Detachment. Accessed July 3, 2019.
Retina Health Series. Retinal Detachment. The Foundation of the American Society of Retina Specialists. https://www.asrs.org/content/documents/fact_sheet_4_retinal_detachment_new.pdf. Accessed July 3, 2019.