Branch Retinal Vein Occlusion
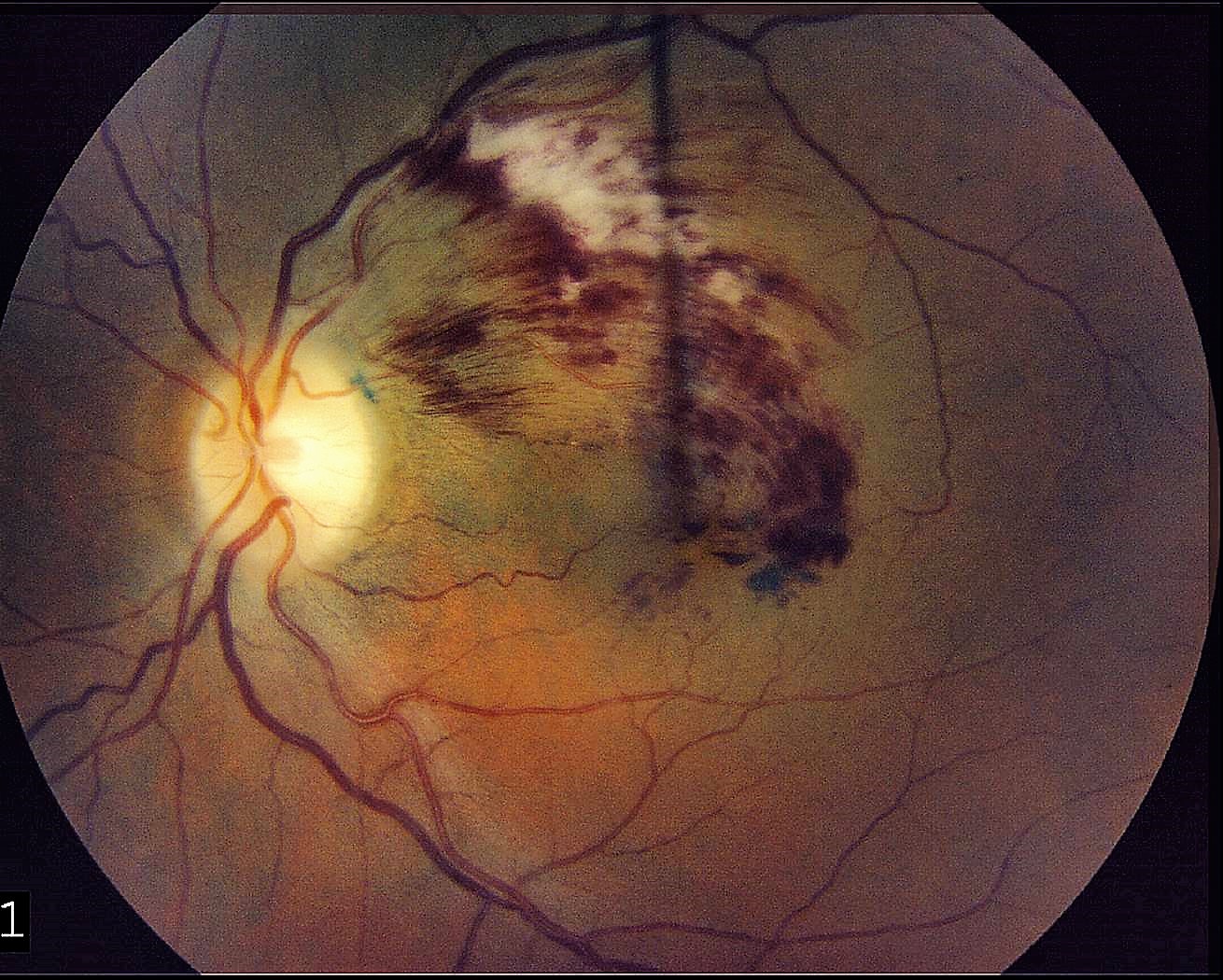
Branch Retinal Vein Occlusion (BRVO) occurs when a branch of the retinal vein becomes blocked, usually occurring where a retinal artery crosses over and compresses a retinal vein. The segment of retina drained by the blocked vein becomes swollen and hemorrhages. The body releases a protein called vascular endothelial growth factor (VEGF) in response to the blockage. This protein causes increased vascular permeability and induces neovascularization, the growth of abnormal blood vessels. Increased vascular permeability leads to leakage of fluid from vessels, and will often cause retinal swelling. Swelling in the central retina is called macular edema, which can result in loss of vision. Vision loss may also occur if abnormal blood vessels grow in the front of the eye causing neovascular glaucoma, or the back of the eye causing vitreous hemorrhage. Ischemia, a reduction in blood supply, can also occur.
SYMPTOMS
Patients with BRVO are often asymptomatic. When symptoms do occur, they include blurred vision from retinal hemorrhage or macular edema. When macular ischemia is present, vision loss may be severe. Spots, strands, or a curtain may occasionally appear due to vitreous hemorrhage. Eye pain caused by neovascular glaucoma may also occur.
EVALUATION
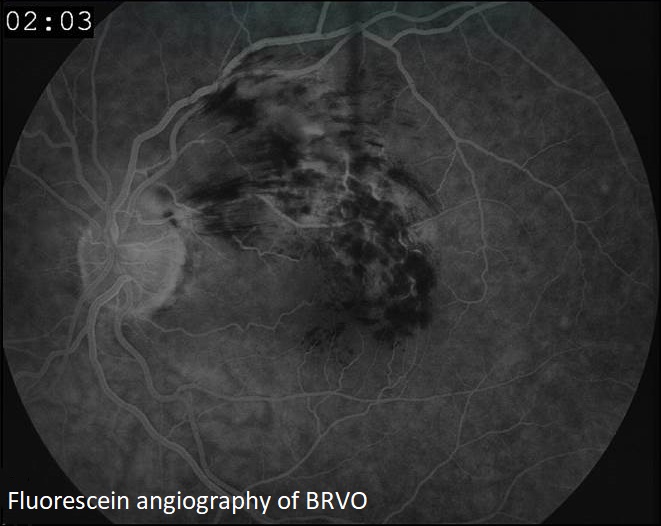
In addition to a dilated eye exam, a fluorescein angiogram may be required. During this procedure, dye is injected into a vein in the arm. Digital images are then obtained of the retina as the dye passes through the eye, making the blocked or abnormal blood vessels detectable to the physician.
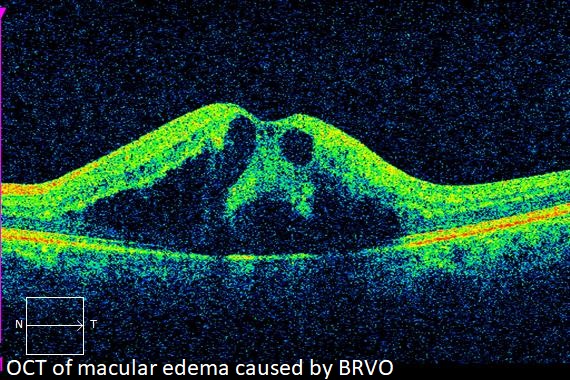
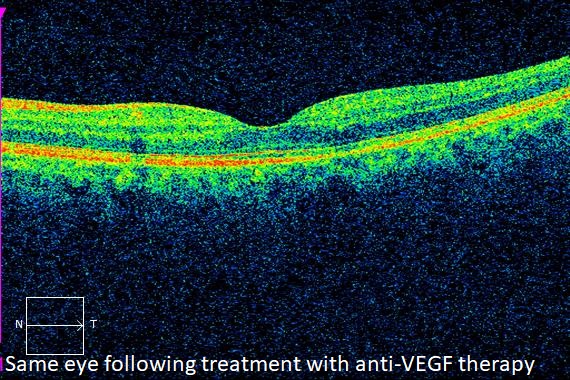
Optical coherence tomography (OCT), a scanning laser that images a slice or cross section of the retina, may be performed to determine if macular edema is present.
Ultrasonography may be used to determine the status of the retina when the view is obscured by vitreous hemorrhage.
TREATMENT
Vision loss due to macular edema often requires treatment. There are three treatments available, which are sometimes used in combination:
Intravitreal injection
Intravitreal anti-VEGF injections are the first line of therapy for the treatment of macular edema associated with BRVO. There are three medicines currently available; Avastin, Eylea, and Lucentis. All three are very effective in causing the edema to resolve and vision to improve.
Usually, injections are performed at 4-12 week intervals, with the frequency decreasing when the condition improves. Cessation of therapy is considered when adequate improvement and stability is observed.
When anti-VEGF therapy proves to be inadequate, second line therapy is often recommended. These include steroid implants or injections, or macular laser treatment.
Intravitreal injections of triamcinolone, a corticosteroid, are effective in reducing macular edema and improving vision. Like with anti-VEGF therapy, the treatment usually requires repeat injections. Steroidal implants such as Ozurdex and Iluvien are also options. Steroids carry a higher risk for cataract formation and glaucoma.
Laser photocoagulation may also be used to treat macular edema due to BRVO. It is less effective than injection therapy, and is usually reserved for cases that respond inadequately to injections alone.
Sectoral panretinal photocoagulation is often recommended when neovascularization of the iris or retina occurs. It works by reversing the regional retinal ischemic injury, causing a reduction in VEGF release. This results in regression of the neovascular fronds.
Vitrectomy may be indicated in patients who develop vitreous hemorrhage. During this surgical procedure, the vitreous gel and blood are removed, and microscopic forceps are used to remove scar tissue. Leaking blood vessels are then cauterized with laser. This is an outpatient procedure performed at the surgery center under local anesthesia.
COMPLICATIONS
Complications of intravitreal injections are well known. They include infection, vitreous hemorrhage, and retinal detachment. In addition, steroid medications carry a greater risk for glaucoma and cataract progression.
Laser photocoagulation risks include bleeding and extension of the laser scars over time.
Risks associated with vitrectomy include retinal detachment, vitreous hemorrhage, cataract, and infection.
Careful technique can decrease, though not eliminate, the risk of a complication occurring.
From the Expert…
BRVO is a disease of retinal circulation which may affect a patient’s vision. Macular ischemia, edema, vitreous hemorrhage, or neovascular glaucoma all may occur. The disease is more common with increasing age and in patients with hypertension, diabetes, or hypercholesterolemia.
The standard of care requires a thorough evaluation including a dilated fundus exam. Diagnostic tests including OCT and fluorescein angiography are often indicated. In patients with no identifiable risk factors for the disease, a workup searching for hypercoagulapathies is usually recommended.
Treatment usually begins by reducing risk factors for the disease. This includes keeping blood pressure, blood glucose, and cholesterol levels under good control.
When vision threatening conditions such as macular edema or neovascularization develop, ocular treatment is usually necessary.
This begins with injections of anti-VEGF agents. Steroid injections or steroid implants are offered as a second line treatment. These pharmacological therapies are sometime supplemented with laser photocoagulation.
The outcome of therapy is usually quite good, with the majority of patients achieving significant improvement in their acuity.
ADDITIONAL RESOURCES
American Academy of Ophthalmology Retina/Vitreous Panel. Preferred Practice Pattern® Guidelines. Retinal Vein Occlusions. San Francisco, CA: American Academy of Ophthalmology; 2015. Available at: www.aao.org/ppp.
Abdelaziz, M, Rostamizadeh, M, and Ahmad, B. Branch retinal vein occlusion. American Academy of Ophthalmology. EyeWiki. https://eyewiki.aao.org/Branch_retinal_vein_occlusion. Accessed July 24, 2019.
Retina Health Series. Branch Retinal Vein Occlusion. The Foundation of the American Society of Retina Specialists. https://www.asrs.org/content/documents/fact_sheet_17_brvo_new.pdf. Accessed July 24, 2019.
Summary Benchmarks for Preferred Practice Pattern® Guidelines. Retinal Vein Occlusions. American Academy of Ophthalmology; 2018.
Ehlers et al. Therapies for Macular Edema Associated with Branch Retinal Vein Occlusion: A Report by the American Academy of Ophthalmology. Ophthalmology 2017;124:1412-1423.
